Mutual of Omaha Collaborates with Lumeris to Enter Medicare Advantage Market



The Supreme Court ruling on the Affordable Care Act in 2012 allowed states to opt into Medicaid expansion, leaving each state’s…
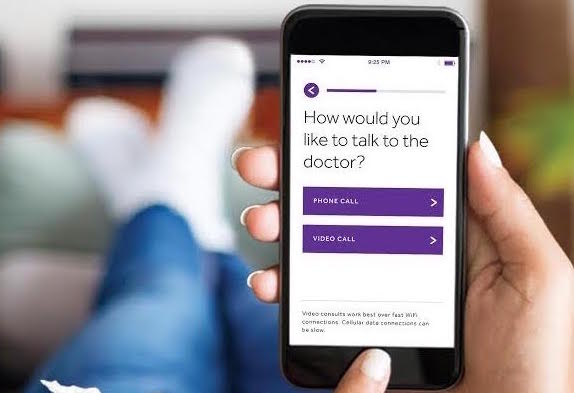
New executive post aligns with Teladoc’s industry leadership and continued expansion Teladoc, Inc., the nation’s leading provider of telehealth…

Solution Provider Offers Advice for Choosing an Enterprise Imaging Platform; Unveils Downloadable White Paper, “Accessible Images, Stronger Outcomes” One…

Hospital operations leaders in emergency departments balance more monthly requests and scheduling rules than any other medical specialty, according…

Illinois-based hospital leverages CarePort Interop to deliver real-time alerts to a national network of post-acute providers, physicians, and suppliers…