VisiQuate Announces Expansion of its Payer Action Center that Can Help Providers Reclaim Millions in Unpaid Claims



American Rheumatology Network announces partnership with Augmedix to scale the use of Augmedix to community rheumatology practices across the…
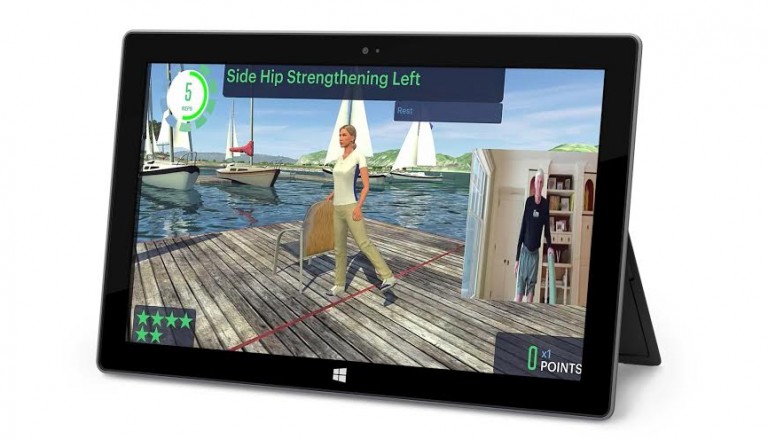
Clinician-Supervised, At-Home Rehabilitation Program Delivers Personalized Physical Therapy Regimen and Outcomes Tracking Zimmer Biomet Holdings, Inc., a global leader…